The Benefits of Wideband Tympanometry

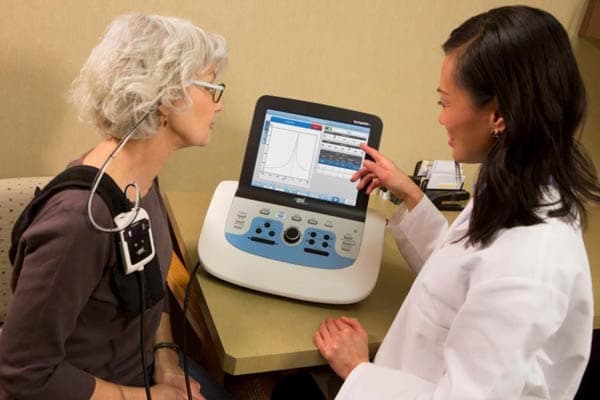
Tympanometry, a diagnostic procedure used to assess middle ear and eardrum mobility, has been limited by its reliance on a single tone. However, with the introduction of wideband tympanometry (WBT), which uses a broader range of sound frequencies, we can gain a more comprehensive understanding of middle ear health.
What is WideBand Tympanometry
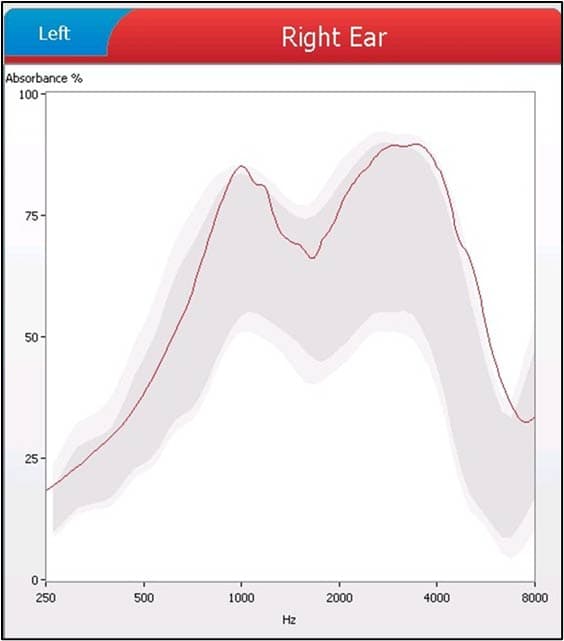
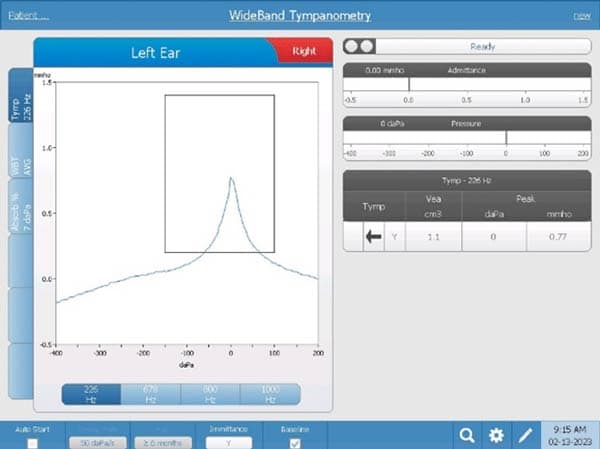
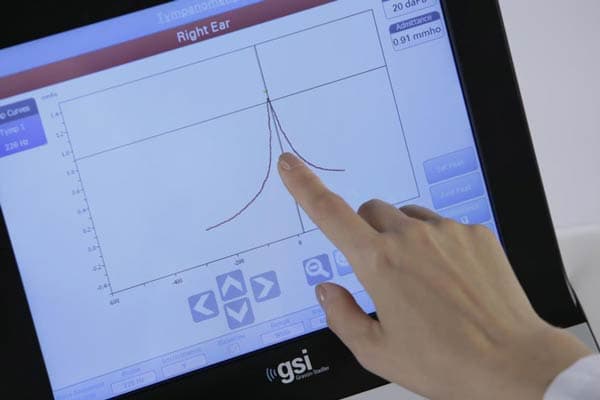
Wideband tympanometry is an advanced diagnostic technique used to assess middle ear function and health by using a broader range of frequencies. Unlike classic tympanometry, which typically uses a single tone (e.g., 226 Hz) to evaluate the middle ear, WBT utilizes multiple frequencies across a wider spectrum, typically ranging from 226 Hz to 8000 Hz or higher.
This broader frequency range provides more detailed information about the middle ear’s response to different sound frequencies, allowing for improved diagnosis of middle ear disorders such as fluid in the middle ear (effusion), Eustachian tube dysfunction, and otosclerosis. Wideband tympanometry offers enhanced accuracy and sensitivity compared to traditional tympanometry, making it a valuable tool in audiological assessments and treatment planning.